In this birth story podcast interview, mom Lacie tells of past infertility and how they discovered a subchorionic hemorrhage early in her 1st pregnancy, but the bleeding never fully resolved. Despite feeling “out of the woods” at her 20 week anatomy scan, Lacie’s water broke and she delivered her daughter, Summer, via vaginal birth at 20 weeks and 5 days. Summer died either prior to delivery or during delivery.
Disclosure: Some of the links within these show notes are affiliate links, which means that if you choose to make a purchase, we will earn a commission, which helps support our show. This commission comes at no additional cost to you, our wonderful listener!
In this episode, Lacie tells us:
- About her infertility journey and being surprised with her first pregnancy after they had given up
- How a subchorionic bleed and eventual weakening of the sac, likely caused her water to break at 20 weeks
- Summer’s delivery and their time together in the hospital together
Listen to all of Lacie’s episodes:
Listen to other stories of infant loss:
- Mom Jan tells of her eclampsia, and the birth and death of her daughter Alice
- Dad Scott recounts Alice’s birth and how she had necrotizing enterocolitis
Full Transcript
Introduction:
Lacie 0:00
Summer Brynn.
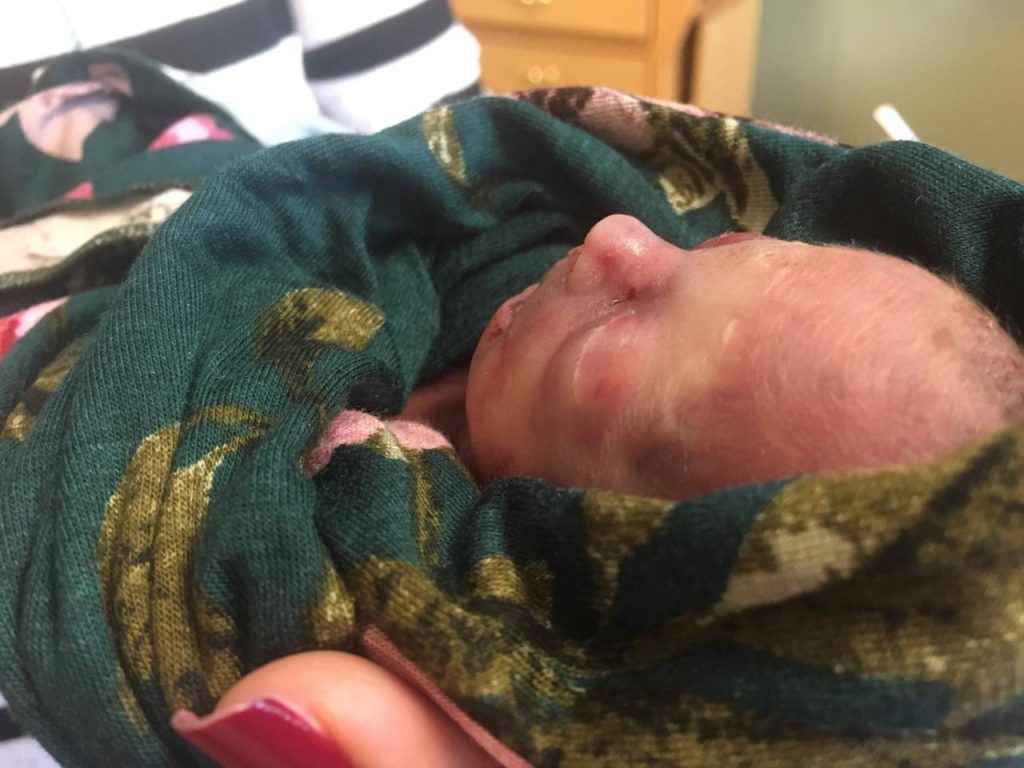
I remember her being so, so very tiny. I could not believe that you could have such perfect features and be so small. I mean, I remember, because their mouths kind of stay open, she had the tiniest tongue. You could see her gums. Her fingers already had fingerprints. Her feet had toe wrinkles. I just couldn’t believe you can be so small and so perfect.
Winter 0:39
Welcome to Still A Part of Us, a podcast where moms and dads share the story of their child who was stillborn or who died in infancy. I’m Winter Redd and on this episode, Lacie is telling the story of her daughter, Summer, who was stillborn at 20 weeks.
As a word of caution to our listeners, this story contains emotional triggers of stillbirth and infant lossKeep yourself emotionally and mentally healthy and seek help if needed. Also, be aware that these birth stories may differ from his or her partner’s, as these accounts are told from their own perspective, through the lens of trauma, heartache and the passage of time. Please respect our moms and dads who are brave and gracious to share their children with us.
About Lacie and her family:
So Lacie, tell me a little bit about yourself. What do you do on a day-to-day basis currently and actually at the time of Summer’s birth?
Lacie 1:33
So I am a pharmacist I work in the ICUs. I’m also typically very active. I like to weight lift mountain bike, I like to garden in my yard. And I do have two daughters, one who will be forever sleeping, whom we’ll talk about, and one I’m so very lucky to be carrying now.
Winter 1:56
To give us some context, how long ago was Summer born?
Lacie 2:00
So Summer was born just over a year ago on June 20 2018.
Winter 2:05
So yeah, just very, very recently. And tell me about your family before this birth. Who’s in your family?
Lacie 2:13
So before Summer was born, it was just my husband and I. We had been together for 10 years already. Prior to having Summer, it was just us the whole time because we were so focused on being active, developing our careers, and trying to build a stable life before trying to have kids.
Lacie’s infertility and pregnancy:
Winter 2:32
Okay, and what was pregnancy like when you did get pregnant? Or can you give us a little background of how your pregnancy went? Any issues with fertility, that type of thing?
Lacie 2:43
Yeah, so this this pregnancy was a long time coming. Before we got pregnant with Summer, we had tried to have her for two years. So during this time, we were diagnosed with unexplained infertility and I really, really struggled with this at that time. After such a long struggle and having no answers, we had both totally given up on having our own child.
Winter 3:08
Thankfully, we did eventually get pregnant with her. And although she was the greatest surprise ever, I really did have a sense of doom the moment I realized I was pregnant.
Why?
Lacie 3:22
I really don’t know why that I–it was just a gut feeling that I had. My excitement was super reserved. I had a deep feeling that even though we tried so hard to have her, that I was going to lose her. Just something about the gut.
And so unfortunately, very early in the pregnancy, at 8 weeks we started having immediate complications. I was at work and I had a massive hemorrhage. And unfortunately, this was over a weekend and I didn’t want to go to the emergency department. Being a pharmacist, I knew there was basically nothing they can do for me. And so we waited over the weekend I assumed I had miscarried and lost her, just like I expected. But that Monday, of course, we got into the doctor as soon as possible. And when I saw that screen, and there was a little beating heart, it was so incredible.
Winter 4:24
Oh, like a huge relief, I’m sure. And, but also a little concerning, because you’re still bleeding?
Lacie 4:33
Yes, definitely. So I had this complication lasted a long time when we were in with the physician, what we discovered was that I had something called a large subchorionic hemorrhage. And so this is a bleed that exists between the sac and the uterine lining. And so this can be quite dangerous, because it can rupture the sac and often leads to miscarriage.
So, of course, me being a pharmacist, I immediately started reading numerous studies on specifically the large subchorionic hemorrhages. And yes, a lot of them did result in miscarriage. But something about stillbirth stood out to me. It just burned into my conscience. And so at that point, so we were eight weeks, we went on to have weekly visits. And even though she was doing fantastic, my bleed was not resolving, as you would expect.
Winter 5:37
Right. So to give our listeners a little bit of information about this type of bleed, do they expect it to resolve? Do they expect it to clot up? What do they expect to see usually?
Lacie 5:50
So what they hope to see is that the blood does start to clot up and then they’ll see it on the screen become old blood. It’s clotted, and then over time, it becomes smaller and smaller. They want this to be resolved by 12 weeks, so by the time you enter your second trimester, because at that point, you start having higher risks. And so, come 13 weeks, mine looks like it’s getting smaller, and then it re-bleeds. So I have hemorrhages again, and it’s fresh blood. And this keeps happening. It goes back and forth, back and forth up until 13 weeks. And this is when my physician says she is incredibly concerned. She wants me to be strict activity restrictions at this point,
Winter 6:37
And up to that point, were you were you being as active as you had been? Because like you said, you really–you work out, you go out you mountain bike, you do all of these things. So you were not really doing anything to restrict that at this point, is that right?
Lacie 6:51
So when we, I found out I was pregnant pretty early, so maybe about five weeks. So from five weeks to eight weeks, I continued weightlifting as usual. Plus you feel good still. But once I bled, we were–I was being more moderate, for sure. So I’d basically not been weightlifting, it was easier exercise at the gym and stuff so that we could try to get this to resolve. And the physicians were okay with that, because they expected that it would resolve. And other women can be active and they totally resolved. But in my case it didn’t.
So, after 13 weeks, we went to strict activity restrictions. And it actually did start to resolve. So it stopped re-bleeding, however, the problem is, is that it’s still, because it was so large, took a long time to clot up and go away. So, finally about at my, right at my 20-week scan, it actually showed that they could no longer see it. So of course someone else is doing your 20-week scan, the MFM providers. They were like, We don’t even notice it; I wouldn’t have even known where this was. So, I got the all clear and for the first time ever, I thought for sure I was going to have this little girl.
Winter 8:18
You kind of breathe a sigh of relief at 20 weeks, at that 20-week scan. So not with your–the people that had been really monitoring it very closely? Just at the regular scan, everybody goes in and gets at 20 weeks.
Lacie 8:31
Yep, the anatomy scan.
Winter 8:32
Okay. And at the anatomy scan, how’d she look?
Lacie 8:35
Fantastic. We just, we really did have the all clear. I got super excited. I had clothes in online carts basically, swaddles, everything ready to go. And I thought I was so safe. And I ordered everything that I wanted for her that night.
Winter 8:57
Then what happened?
Lacie 8:59
So, at 20 weeks and five days, this is when I would say that my world shattered. And so I had just gotten out of the tub when I felt a gush of fluid. And because I had just gotten out of the tub, I was clean, all of that, I knew in an instant that my water had started breaking. It wasn’t very much, but I just knew that that’s what it was going to be. I was super numb, and even though I knew it, I tried to ignore it.
This is fairly late at night, and I even tried to go to bed without telling my husband that anything had happened. But while I was in bed, I felt another little gush. So I told my husband, Hey, I think there’s something wrong. But given all that we’ve been through, I didn’t want to overreact. Maybe it would be okay. It was something stupid. We weren’t going to go to the hospital. But I told him if it happens again, we have to go. So, unfortunately, just before midnight, I felt a third little gush. And I told my husband, It’s time to go. We were up and go on in moments. He didn’t question anything about it. It’s like, he just knew he had to listen to me.
And so when we get to the hospital, we’re standing in front of the L&D desk, and my water breaks completely. It’s just coming. Totally wet. Soaked. That, that was definitely my water breaking. There was no more denying what had occurred at this point.
So they take us back to a room, of course, to see if this is your amniotic fluid, what’s going on, all that sort of stuff. And during my workup, of course, they do an ultrasound. And they can see there’s no, there is no fluid. She can’t move out all. She’s no longer that wiggly little baby that we saw 20 weeks.
Winter 11:04
And you were able–you did see her move. And did you feel her move up until that point?
Lacie 11:09
Prior to this, yes. Yep, we had seen her moving. I felt her moving. And now here she was on the screen, completely immobile, because all of the fluid is gone. But I can see her tiny heart beating. Basically, I know that this is the last time, I’ll ever get to see her heartbeat. And it was it was just, I’m watching her and I know she’s alive. And I know that I’m going to lose her.
Winter 11:40
What did the doctor say? What did the, I guess, the intake folks say to you when they said you’re 20 weeks and you’re, you have no more amniotic fluid? What did they say?
Lacie 11:51
So, of course it’s midnight and it’s just the on-call physicians, so I don’t even have my physician there. But they come in and they tried to explain what they thought had occurred. And I definitely agreed with them. And the thought was that this subchronic hemorrhage, which again bleeds up against the sac–blood is inflammatory–and so because it had occurred so many times and lasted for so long, the thought is that all of the inflammation and the bleeding caused her sac to weaken. And so, of course, as she got bigger as she moved, it was too much to take.
Winter 12:35
Yeah, and there is enough–there’s a pressure point basically then kinda broke.
Lacie 12:40
So at that point, my sac broke and there is nothing you can do about that.
Winter 12:46
Yeah. So what were the options that they presented to you at that time?
Lacie 12:51
Yeah, so they they did lay out all the options that I had for a pregnancy nearing 21 weeks. I was 20 weeks and five days. Basically what they said was that I can try to keep her in essentially. Hope that I don’t go into labor, and then they would deliver her at 23 weeks and try to take care of her in the NICU. The problem with this is that she has no amniotic fluid. And so before you even get to 23 weeks, you’re already inducing complications, in that, she would develop muscular strictures. And because the amniotic fluid is gone, she would already be developing lung issues.
So as the physicians are telling me all of this, I’m barely listening at all. I am a critical care pharmacist, and even though I didn’t train in pediatrics, I kind of knew all that I needed to know about a pregnancy this early. But the problem was that my husband does not have a medical background. And I knew right away that I didn’t want him to regret anything. And so even though I wanted the physicians to stop talking, I had to let them finish their entire spiel basically of our options, because I needed him to know what the consequences were of a 21-week delivery at that point.
Winter 14:25
And did they spell that out pretty well for him? Like I, I’m curious to know if he was acknowledging this because when you get news like this, your brain, at least, my brain shut off. You’re like, what? No, no. So how, how did he handle that?
Lacie 14:44
So, in my perspective, I think really what was occurring is that he actually just trusted me. On the car ride to the hospital I told him, we will lose her. If my water is breaking, there’s no going back, and we will lose her. So I was still listening to the physicians. It was kind of like, yeah, that’s in line with what I’m thinking. Yeah, yep. No. I don’t want this. I don’t want this. I don’t know if he was able to absorb all of that or not. I mean, I had to allow him the chance to absorb it. But I think in all reality, it came down to, he knew that this was something he couldn’t question me on. That I knew this in my heart, and there was no going back on this.
Winter 15:36
Yeah. So what decision did you end up making?
Lacie 15:41
So after all of this after talking, the physicians didn’t even wait to really hear answer. They more just said, we’re going to allow you some time to talk it over. We’re not going to sit and debate this right now. We’re going to let you talk this over as a couple.
And by now I am wanting out of this little tiny ultrasound room. I’m over it. I know my choice. I do not want them to leave me in this room any longer contemplating choice that I don’t have. And so I ended up stopping them immediately. And all I did was look over at my husband with a face of “you know, there is no discussion.” We’re not discussing anything. We do not have a choice. And all I could do is turn to the physicians and say, No, I cannot do this to her. And that was my answer at that point. To me, unfortunately, at 21 weeks for my little daughter, I decided that death was going to be better than life in the NICU for her.
Winter 16:55
A long stretch in the NICU if she gets out. Okay, so what happened then? Tell us about the delivery. What? What occurred after that?
Lacie 17:07
So for me, I chose to actually be induced right away. So as soon as they got me to my room, we started labor. To me, my little girl, she was alive. Her heart was still beating.
Winter 17:23
Yeah. And they had a monitor strapped on you the entire time. Okay.
Lacie 17:26
Yep, they did. And I just, I could not bear the idea of going home to wait for her to die. Because they, yes, they gave you, sure, you can try to wait until 23 weeks. But I knew that this little tiny baby is not going to survive to 23 weeks and I wouldn’t want to save her at that point anyways.
So at this point, my OB-GYN and I had not even discussed delivery yet. This was an my first child, and I had no idea what delivery was going to be like. And because I was so concerned with her the entire pregnancy, I was not looking at researching delivery and stuff yet, because those were not considerations I needed yet. We had other things to deal with. And so, so I had absolutely no idea what I wanted my delivery to look like. And the nurses are asking you what, what are your preferences, and all that sort of stuff. And I have no idea, but being the I’ve worked with palliative care, and I work the critical care units and stuff, I knew what I wanted, at least from that perspective.
Winter 18:45
Okay. So you explain your preferences to the team. Your husband, Eric, did you guys talk that over and kind of how you wanted, because the nurses are kind of sending a barrage of questions of like, what you want and how it’s going to look and that type of thing. He’s probably–are you helping translate what it’s going to look like?
Lacie 19:06
No, because I have no idea. So he he had no input on it. Honestly, biggest question, I think that I remember was, do you want an epidural? I was like, Well, I have no idea. I don’t know. I would have liked to have gone natural, but I don’t even know what I’m going to experience or anything like that. So I had no idea.
Winter 19:31
Yeah. Did you end up deciding on an epidural then?
Lacie 19:34
So my epidural was actually quite a traumatic experience. So basically, we waited for quite a while before I felt what I would have realized as a first contraction. Of course, they’re telling you you’re gonna, you are contracting and all that but, I don’t know.
Winter 19:55
First time, never talked about it with your right your provider.
Lacie 19:58
So now I’m starting to notice, Okay, I’m having a contraction. But because I’m being induced, this contraction never goes away. I’m actually asking my mom and my sister, like, when do I get a break? Because everybody else gets a break from their contraction. No, this doesn’t occur for me with this induction. I end up going into a full body spasm and they’re trying to give me fentanyl pushes, some pain medications. And it works and I kind of say, well look if this keeps me calm on up, I don’t want the epidural. And at this point, I don’t even know how long labor lasts.
Winter 20:41
Yeah. Now let’s give a little bit of time frame now. You guys arrive at the hospital to get checked out probably what one o’clock in the morning or so.
Lacie 20:50
Yeah, right after midnight.
Winter 20:52
And you guys make the decision. When was–when did you get started? Like two in the morning, three in the morning?
Lacie 20:59
No. So all of this took until about 6:30. It was right before shift change for the nurses.
Winter 21:06
So you guys got checked in, all of that stuff and then got started around 6:30 in the morning, okay. And then, so you’re kind of progressing. You’ve had some pain, you’re noticing some contractions, and how long? When does that hit or so, that you can remember?
Lacie 21:22
So this would have been probably about three o’clock now.
Winter 21:26
Okay. So it’s been going on for a little bit. And then–
Lacie 21:31
Well, three o’clock is when I first noticed a contraction. It moved, my delivery was very fast in that regard. So from first contraction, I start spasming up, and it’s actually everybody else that’s kind of freaking out. They want to give you pain control, and they don’t want to see you in pain. But if they had talked to me through it, of you know, you’re actually going to be incredibly close, I would have preferred that I never got the epidural, because it took, because I was in a full body spasm, it took three people to roll me over for the anesthesiologist. And of course, that didn’t go well.
Winter 22:15
right?
Because you’re in a full body spasm!
Lacie 22:19
So the epidural never works. And they decided, well, let’s roll her over and see if it drains out. So they, three people again have to take me in a full body spasm, rolled me over, and they’re trying to adjust this epidural. And I just at this point, I wish that they would have just said, No, you’re so close. This is ridiculous. That was basically the only traumatic thing about my delivery.
Winter 22:47
It sounds like your family, your sister and your mom are there. Eric, your husband Eric is there as well. Anybody else in the room there?
Lacie 22:58
No. So going back to what it looked like when we first started this induction process, I knew that I wanted my parents and my sister to be there. I certainly didn’t want a lot of people to be there. That was never how I intended a delivery to be. I just wanted it to be private. But I knew that they wanted this baby just as much as I did. Absolutely. And this wasn’t going to be a normal delivery. So I called them early. I didn’t bug them at three in the morning. So for them, it’s kind of a big surprise, that I’ve been in the hospital all night. But they came in and delivery, or at least, the whole induction labor process was very calm up until we started the contractions. I was still super numb. I wasn’t super emotional yet. And I couldn’t process what this ultimately meant, it was kind of like we were just going with the flow of something that was inevitable and I didn’t quite grasp what this was all going to mean in the end.
Winter 24:13
So what happened during the delivery then? So you’ve it’s close now and now eventually it will be time. So what was happening then?
Lacie 24:22
So for me Everything was super–to me, everything was super chaotic, because people were trying to roll me over. People were trying to give me pain control, instead of us talking through the actual delivery!
Winter 24:35
–what to do! Did you, I’m actually curious, did you express that? You’re like, I don’t know what to do.
Lacie 24:41
No, I was so I couldn’t even talk. I was just in this painful body spasm and everything was kind of blacked out at this point. And people were just chaotic around me. And I was just like, I don’t even care. I’m just I, like someone just hold my hand or something. Don’t play with my epidural! Don’t, don’t, don’t touch me Don’t keep trying to reposition me. All that sort of stuff. Ultimately, though, my total labor and delivery was very short. It was an hour and a half from the time I felt my first contraction until the moment she was born, so that’s why it’s so fast and chaotic. I don’t know if they even expected it to be so short.
Winter 25:38
So you were, they were checking you, I’m sure the entire time, making sure. And then, so they did notice that you had progressed very quickly in that short amount of time.
Lacie 25:46
Yeah. So I do know, even though I was kind of in this blackout state, that my family had left the room. I mean, of course it’s getting chaotic. And in fact, she’s tiny right, she’s coming. She’s actually coming out sideways. And the nurses can’t deliver her and my OB-GYN was still in the process of coming up from the clinic downstairs. And so it is getting super chaotic. My family left. Once my physician arrived, I could tell that unnecessary staff had left, because at this point, it’s finally getting quieter. Basically, there’s not as much yelling going down and all that sort of stuff.
So I deliver my daughter. And the moment she was born, it was just complete silence in the room. And so I knew that with the silence–I wasn’t necessarily expecting her to cry–but I knew what the silence that my physician was waiting to see if she was going to take her first breath. And when it was so quiet during those first couple moments, I knew that she was watching my baby to see for a first breath, and she didn’t make it. So we didn’t, I didn’t want to know, through delivery if she had passed away or not. We were just going to wait until labor and delivery. And I just I knew she hadn’t made it.
Time with Summer after delivery:
Winter 27:24
How were those moments together though after?
Lacie 27:26
So right after, of course, it felt like forever while they were holding her and getting her clean and all that sort of stuff. It felt like forever. But as soon as they placed her in my arms, it was just a ton of crying. Tons and tons of crying. Who knows how long it went on for? No words could be spoken at all. I just know that. It was kind of nice in that everybody just stopped and cried and didn’t interfere with anything. You know, the nurses and my OB-GYN are crying me and my husband, of course, are crying. It was just completely overwhelming, that you’re sleeping baby has been put in your arms.
Winter 28:15
Yeah. Yeah.
Lacie 28:18
Eventually, after things settled down, I told my husband that he could go and get my family. So that we could all be there. Again. I didn’t know what I wanted for delivery, hence, so it was super chaotic and not fun. But from a palliative perspective. I really knew what I wanted. In my career, I’ve been around a lot of death. And it’s something that’s inevitable, and I wanted it to be as peaceful and as happy as possible. So for me, I wanted to savor every single moment I was going to have with her because I knew it was going to be short.
I wasn’t going to be able to develop all these memories with her, so that’s just exactly what I did for the short time that I had her. I just remember, I just wanted to caress her and touch and look at every single tiny feature of her. It’s kind of like I was hoping to burn her into my memory, so that I knew what it was like to be touching her fingers and toes and her nose and her lips and all that sort of stuff.
And then I definitely, even though I wanted to hold her and hug her, there was also this component of, I wanted to see her. So of course you’re holding your baby, it’s kind of hard to see them. You want, you want that weight of them. You want to feel them. But at the same time, I also want to see her and this is where I took advantage of, you know, my husband was holding her, cradling her. He was transitioning into becoming a dad.
I wanted to soak that in. I just wanted to see and feel the love that other people had for her. So I definitely just sat and admired what it was for him to look like as a dad, because we had waited for this for so long, right. And it was the same with my mom. She had waited for this baby forever. And I know that my mom, of course, she was going to get a short time, very short time with her. My mom was holding her as much as she could. And whenever she did hold her, she never ever, ever looked away from her face. And so I just, I tried to really soak that up.
And then obviously, I just, I really can’t put into words what it was to have her. I knew that she was sleeping. But to me, my heart, my arms, they were all so full at that moment. It’s like she wasn’t gone yet. at that point. I only got to spend four hours with my baby.
Winter 31:05
And was it, that–was that your choice to spend it, only four hours?
Lacie 31:10
It was that we had come in overnight. And by the time, we had her it was 4:30 in the afternoon all that sort of stuff. And we were, we were becoming incredibly exhausted. We had had no sleep at this point for almost 48 hours, 36 hours. It was, it was just becoming tiring and hard. And I didn’t want–I know they have the cots and stuff that can cool them–but I didn’t want to sleep in the hospital and have her in a cooling cot and all that sort of stuff. So we chose to just soak in what we could and when it felt appropriate, it was time to go home without her. But every single, even those four hours, every single moment with her meant the absolute world to me. And it’s when I realized that she was truly worth all of the pain in our pursuit to have her.
Making memories with Summer:
Winter 32:17
So during this time when you were with her, did you have pictures taken? Did you have any molds done of her hands and feet? I’m actually curious to what you did, so that you could have a few things to hold on to.
Lacie 32:30
Yeah, I mean, when you, when you have a baby that is born sleeping, again, you don’t get to develop and make those memories. And so every little bit is worth it. I remember the nurses said take pictures. They actually encouraged take pictures because it does feel morbid. And you kind of want to actually just spend time with them versus taking pictures, but I’m so glad that we did. I definitely tried to take close-up pictures of all of her teeny tiny features. And I was, I was the one actually sitting and taking pictures. You know, it wasn’t other other people. And so I was taking photos of my husband holding her, so that I would not forget this. And I have a photo of my mom just staring at her face. And so those, those are there.
Winter 33:28
Good. And did you do molds as well?
Lacie 33:31
We did. So they took her and did molds. And I am very glad that they did that. Because even though I remember her being so tiny, just last year on her birthday, I went back to her molds. And it’s insane to actually see and feel again of how small she really was.
Winter 33:56
Yeah. I’ve seen pictures of them and they are tiny, they’re just tiny little hands and–
Lacie 34:03
–super tiny. But yet these molds still show her fingerprints and all those toe wrinkles and stuff like that. So those are very nice momentoes to have.
Naming Summer:
Winter 34:14
That’s great. So during this time, you’re close with your family. You’re close with your husband. You get time together. At this time, is this one you guys named her? Or did you decide? I don’t know when this, I actually don’t know when you named her Summer.
Lacie 34:31
So yes. It’s actually a story that lasts the entire delivery process the entire day. My husband and I had discussed names beforehand, and we did have two strong names in the running. But again, for us, we had other things to worry about right with this pressure. And so we just ultimately decided that we would wait until delivery to decide her name to see what she looks like see what she’s meant to be. Well, now here I am, in a very unexpected situation having to make delivery plans, choose her name and make cremation arrangements in one–all at the same time.
Winter 35:17
Yeah, I was going to say in less than, what, 12 hours, basically?
Lacie 35:21
So you’re having to make all of these decisions. And before I started going into labor, the nurses asked, so they could put it on the board, What was her name going to be? And at that point, I didn’t know. I realized, I was just super crushed. I realized that I had no idea what her name was going to be. And this was not how I envisioned choosing her name. You envision a very different moment if you’re gonna wait until delivery to see the personality of your baby, what they look like, all that sort of stuff. But I didn’t know. And so, thankfully, they didn’t ask again until after delivery. But very shortly after she was born, the nurses again asked, What was her name? And at this point, I can’t even respond. I’m just crying. Winter was actually my favorite name. But I kept looking at her. And it did not fit. It was not a fit at all. I felt like I couldn’t, even though it was my favorite name, I couldn’t force it upon her. So thankfully, they let it go.
Some time passes. But they again, come back and ask had we decided on a name yet. It’s like everybody just gets so obsessed with the name when you’re in delivery and stuff like that. And I didn’t know, I didn’t have the strength to decide her name. To me, that was just such a huge decision to make. I can’t deal with this right now.
But thankfully, this is when my husband actually spoke up. And he just said that her name was Summer. This is not a name that we had ever, ever once brought up. Not once. So like, Where did that come from? But he just went on to say that it was the summer solstice. And if we named her Summer, we would always remember her when the summer solstice came around. Now it’s actually kind of funny, though, because June 20 is not the summer solstice. But it’s not like we knew what day it was anymore, so it just makes it all the more funny.
But as soon as he said that, I did, I looked down at her and it was the absolute perfect fit. Her name was going to be Summer and there wasn’t a question in my mind. I was–we had settled on it very quickly. I had no question of “Are you sure?, “Why that?” We’ve never talked about this before. I just looked at her. It was a fit. And I felt so relieved. So relieved to have a name for her. And I just looked back at the nurse. Her name is Summer Brynn.
Winter 38:13
Oh, that’s so awesome. I just got chills, because I was like, you know, when you I guess when you know, you know? Right. And that was cool. Interesting that Eric was like this is it.
Lacie 38:25
Yeah, it was very matter-of-fact. There was no discussion of “What about this name on the list?”, “Or this name on the list?”, “What about the middle name?”, “Should we use that as a first name?” It was just, these names didn’t fit, and Summer did.
Giving Summer to the hospital:
Winter 38:41
That is awesome and beautiful. So after the four hours that you decided to spend with her, it’s getting to be, I’m assuming, around eight, nine o’clock at night. And you’re exhausted. Tell me about giving her back to the hospital.
Lacie 39:02
So it’s not even…you don’t even kind of say like, Okay, I’m ready. Here she is. They actually came in and asked, Can we go do her molds? And they kind of laid it out there of, some parents can handle having there baby back. Some parents can’t do this twice. And I chose that I couldn’t do this twice. There was only going to be one time that I was going to hand her over. And it was definitely the absolute worst moment of my life, deciding that this was the last that I was going to see my baby, I was going to let go of her. And I was never ever going to get her back.
The finality of this moment is so unbearable, and you can’t believe that you are experiencing it at all. And so I had her swaddle that I–it was like the only thing that had arrived for her at that point. And so I had her in one of her swaddles. And I didn’t want the hospital to take it. I didn’t want it to be cremated with her. It was mine. And so I unwrapped her. And it was hard, because it’s like you’re letting them be unprotected and alone at that point. And I handed her over to the nurse.
It’s hard to like you literally think about your fingertips are letting go of your baby. And that’s it. And then with that, we had been at the hospital for 22 hours. That’s as long as we had been there. And that’s when reality starts to actually settle in, is you hand over your baby, and it’s time to leave the hospital. And so within those 22 hours of arriving there, you’re walking back out of those hospital doors, with empty arms. And you just, you cannot grasp the fact that you have just delivered your child and you are leaving them behind. And you’ll never be with them again.
Winter 41:38
It’s awful. It’s awful. It’s awful. It really is. It’s–that was, yes, that was–it’s awful. And it feels hopeless, actually. Yeah, and it’s not fair, doesn’t feel fair at all, does it?
Lacie 41:54
No. It doesn’t feel natural. It’s not what is supposed to happen in your life.
Winter 42:01
Yeah. Were you feeling okay yourself physically?
Lacie 42:06
Yeah. Surprisingly, I couldn’t believe that I would. They were just letting me be discharged. But physically, I was okay. And safe to go home. And I–there was no way, I wanted to go to the mom and baby floor, because they were going to, they needed to get me out of LND, the delivery room. And that’s part of what made our decision to was that, Yeah, we could stay longer. But that meant going to mom and baby. Yeah. And I wasn’t having that.
Winter 42:37
You’re like, nope. Did you guys go home straight away after that?
Lacie 42:42
straight home and went to bed. Just thankfully, in the timeline, it was time to just go to bed. And you didn’t have to think about it yet.
Cremation and a glass heart:
Winter 42:54
So you mentioned before that in this very short amount of time you are realizing that outcome of what’s going to happen. You get induced, you have a baby, you name your baby. And you mentioned that now you have to talk about cremation services. How was that deciding that?
Lacie 43:16
They just, they give you…thankfully, I had known what I would do in these cases.
Winter 43:25
You had thought about it before.
Lacie 43:26
Right, just more from being my career. Yes. we talked more about it.
Winter 43:31
Yes, we definitely–this is something that we ask patients, right? Some things that patients are asked all the time. And so it should be. It’s always good to have it on our list to take care of, right?
Lacie 43:43
Yes, definitely. Even though I didn’t envision losing my own child, I knew that I would have wanted her cremated. And so we we started that process. And we eventually put her into, her ashes, into a glass heart.
Winter 44:01
Oh, now is that–so you had her cremated? Through–was it, is it like a hospital program? I’m trying to think of how they–they come in and talk to you about it. And they’re like, this is what you can do. And I’m not sure what that process looks like for you.
Lacie 44:18
So they basically just give us a list of funeral homes have it’s not like they even went through the options of “Do you want to bury her?” “Do you want to cremate her?” This was going to be between you and the funeral home. And so we didn’t even go over that. It was just I selected a funeral home. And then we had her cremated. You bring those ashes home, and then you can actually just select a company that does glass, whatever. Glass art. It doesn’t have to be glass heart. And you send their ashes and they incorporate it into a piece.
Winter 44:56
How long did that take?
Lacie 44:58
That was a couple months actually.
Winter 45:01
Probably took some time to, to do all of that. I remember you writing about that, actually. And how unsettled you were not having her close.
Lacie 45:15
Yeah, it was like–yeah, it was like it wasn’t a finalized process yet. Because like saying your case or other people’s cases, you have a burial. And that’s kind of closure. At some point, like, you know that you’ve kind of wrapped up this process. And you know where they are. But because this took so many months, her ashes were just out there. And I hadn’t yet kind of received her back. And so it did it felt like this was not a closed process at all.
Winter 45:50
Yeah. And that was, yeah, once again, unsettled. I’ve got some loose ends.
Lacie 45:55
Yeah. So that was hard waiting for her to come back.
Winter 45:58
Yeah. What do you think of a piece? Like what do you think of the little heart now?
Lacie 46:03
I absolutely love it.
Winter 46:05
I think it’s beautiful. By the way. I wish I could share a picture–I’m not going to because that’s a it’s a very personal thing. But it’s very beautiful. And it’s very, I like that you–it’s there. It’s always there–Summer’s always there. And you you tend to it, I guess is a good way of putting it. You tend to it you give her bows. You give her, you, it’s she’s part, she’s part of your home and your in your lives. I think that’s great. Is there anything else you want to tell us about Summer that you want to remember or call out that we didn’t cover?
Lacie 46:39
The only thing, you know, it’s funny the actually did a–they started stillbirth research the month that my daughter was born, just trying to look into what are the factors behind this and all that sort of stuff. And they asked the same question. And all I just want to say is that I want her to be remembered. I don’t want her to be forgotten.
Outro:
Winter 47:10
Many thanks to Lacie for being vulnerable and sharing your story of Summer with us. It was beautiful.
Head over to our website, Stillapartofus.com, where you can find the show notes including a full transcript of this interview and any resources that were mentioned, where you can sign up for our short and helpful email newsletter, where you can learn how you can become a patron and support the work it takes to produce this show for just a few dollars a month. And lastly, where you can find out how to get in touch with us, if you want to share your child’s story on the show.
The show was produced and edited by Winter and Lee Redd. Thanks to Josh Woodward for letting us use his song “Flickering Flame.” You can find him at JoshWoodward.com. Lastly, subscribe to this podcast and share it with a friend that might need it and tell them to subscribe. Why? Because people need to know that even though our babies are no longer with us, they’re still a part of us.
Andy Rooney
The average dog is a nicer person than the average person.
